It's easy to step on the scale, see your weight hasn't changed in months, and assume nothing has changed.
But what many people don't realize is that most common scales measure only one thing: your relationship with gravity. It doesn't measure metabolic health. It can't detect muscle loss. It doesn't track insulin sensitivity, functional capacity, or chronic disease risk. It can't tell the difference between muscle and fat.
What people rarely consider is body composition: the proportion of muscle versus fat in your body. This distinction between muscle and fat is what can actually be a good indicator of your health outcomes, not the total number on the scale. Consider two people who both weigh 170 pounds. One lifts weights regularly, has maintained muscle mass, and has around 20% body fat. The other has been sedentary for years, has lost significant muscle, and has 35% body fat. Same weight, but their metabolic health, strength, and disease risk are completely different.
Body composition is a very important metric that can help determine metabolic health, functional capacity, and how well you age. Interestingly, the average person loses roughly 3 to 8% of their muscle mass per decade after age 30, often replacing it with fat. The weight might remain unchanged and be the same on the scale, but the body is slowly transforming in ways that can profoundly impact strength, metabolism, and long-term independence.
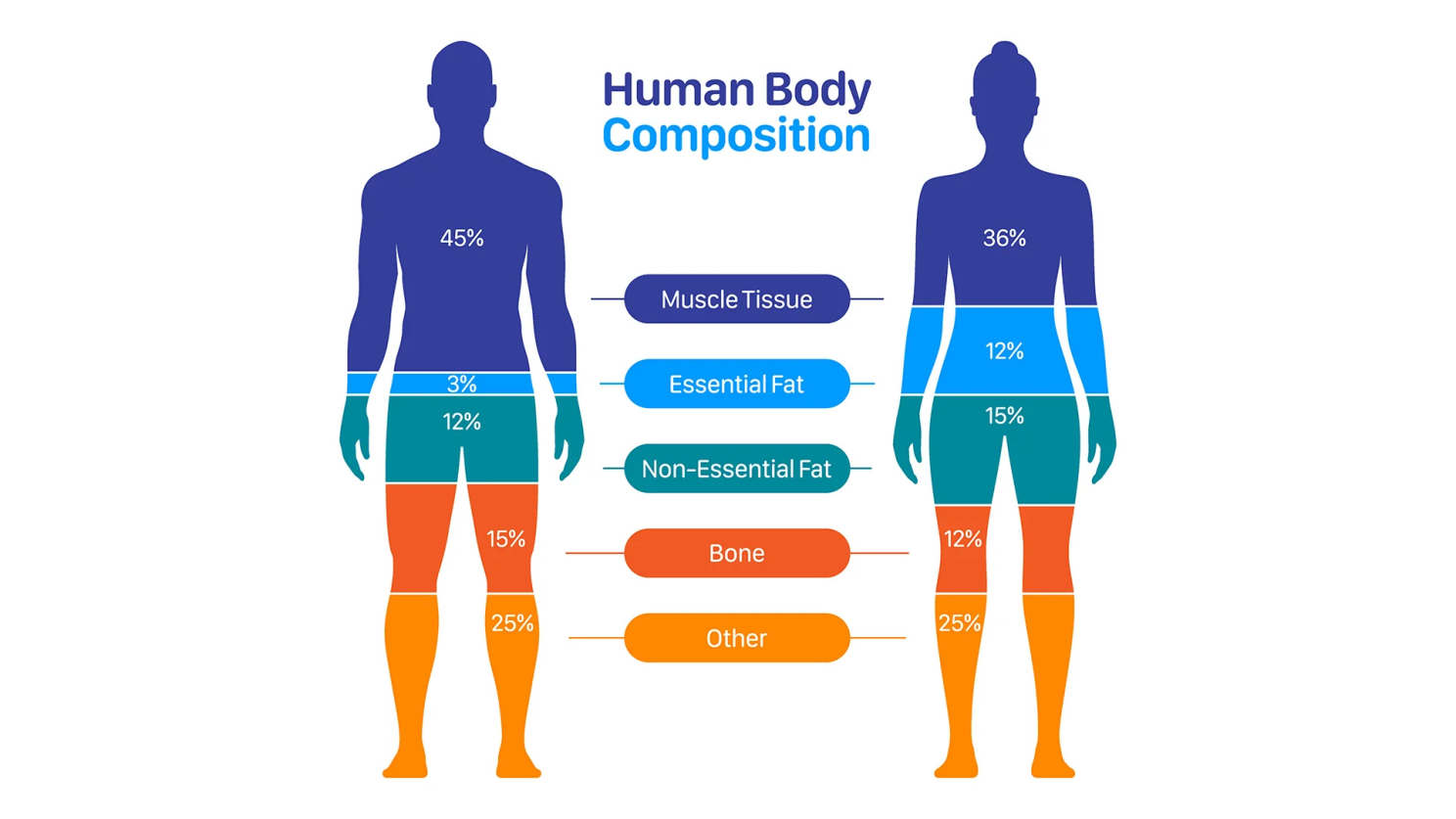
First, we need to understand why muscle matters beyond the obvious. Most people recognize that muscle is important for strength and movement, but the deeper question is: why does muscle mass influence how long and how well you live?
The answer goes far beyond physical appearance or athletic performance. Muscle tissue functions as one of the body's most metabolically active systems, influencing everything from how your body processes glucose to how it responds to injury and stress. When muscle mass declines, it creates a cascade of changes that can affect metabolic health, functional independence, and resilience against chronic disease.
Understanding muscle as more than just the tissue that moves your body reveals why maintaining it throughout life is such an important factor in healthy aging. It's not about building maximum muscle mass for aesthetics. It's about preserving the metabolic, functional, and hormonal roles that muscle plays in supporting long-term health. Muscle doesn't just decline passively with age. Its loss actively accelerates other aging processes. Less muscle typically means reduced metabolic capacity, which can lead to insulin resistance, less mechanical stress on bones that can accelerate bone loss, and decreased functional reserve that can make recovery from illness or injury more difficult. This is why muscle mass is increasingly recognized not just as a marker of fitness, but as a predictor of metabolic health, physical resilience, and independence across our lifespan.
Metabolic Health
Muscle is the primary site for glucose disposal in the body. When you eat carbohydrates, your muscles store glucose as glycogen and use it for energy. Higher muscle mass tends to be associated with better insulin sensitivity, meaning your body can more effectively regulate blood sugar. This relationship may help explain why maintaining muscle mass can support metabolic health and potentially reduce the risk of type 2 diabetes.
Muscle tissue is also metabolically active, meaning it requires energy even at rest. While the actual caloric difference per pound of muscle is relatively small, greater muscle mass can contribute to higher total daily energy expenditure, which may support weight management and metabolic function over time.
Functional Capacity and Independence
Muscle strength directly determines your ability to perform daily activities. As muscle mass declines, routine tasks that were once effortless become progressively more difficult, which can potentially limit independence and your overall quality of life.
Research suggests that muscle strength, particularly grip strength and leg strength, may be associated with longevity and reduced risk of disability in older adults. Maintaining muscle mass throughout life can help preserve the physical capacity needed for independent living.
Myokines and Hormonal Signaling
Skeletal muscle functions as an endocrine organ, secreting proteins called myokines during contraction. Think of myokines as chemical messengers that muscles release when they work, similar to how hormones are released by glands. These signaling molecules travel through your bloodstream and can influence other organs and systems throughout your body.
When you exercise, your muscles don't just get stronger locally. They release myokines that can affect your metabolism (helping regulate how your body uses energy), inflammation (potentially reducing chronic low-grade inflammation), bone health (signaling bones to maintain or increase density), and even brain function (supporting cognitive health and potentially reducing risk of neurodegenerative disease).
This is why exercise benefits extend far beyond the muscles being trained. The myokines released during muscle contraction appear to contribute to many of the systemic health benefits of physical activity, including improved insulin sensitivity, better fat metabolism, and reduced inflammatory markers throughout the body.
Bone Health
Muscle contractions create mechanical stress on bones, which can stimulate bone formation and help maintain bone density. This relationship between muscle and bone suggests that maintaining muscle mass may also help protect against age-related bone loss and osteoporosis (a condition where bones become weak and brittle).
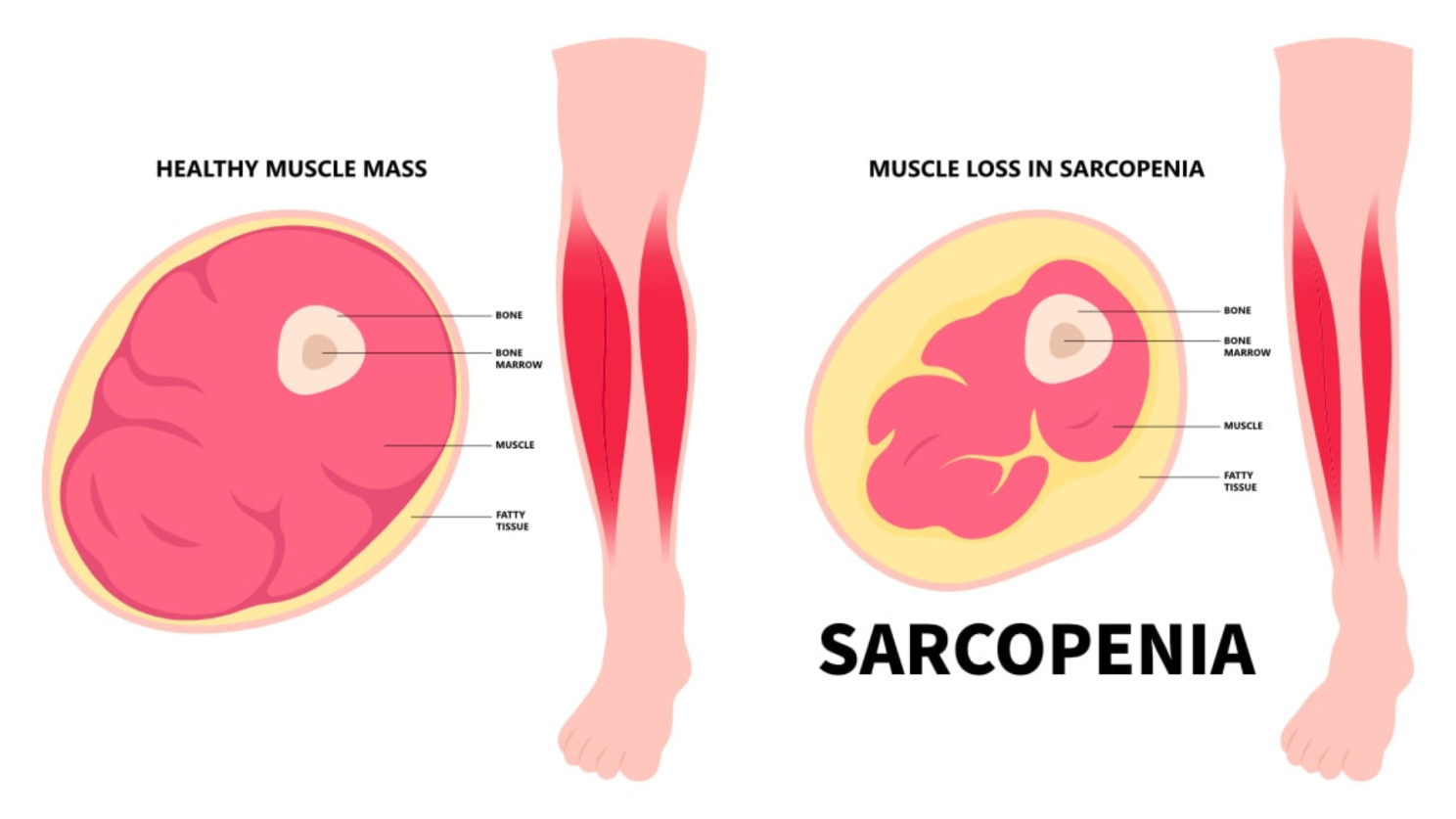
Starting around age 30, adults typically begin losing muscle mass gradually, a process that can accelerate significantly after age 50. This age-related decline in muscle mass and function is called sarcopenia. It's important to understand its role in body composition changes and why it matters for long-term health.
Sarcopenia doesn't just mean having less muscle. It's associated with decreased strength, reduced ability to perform daily tasks, increased fall risk, and loss of independence. The decline can be subtle at first, progressing slowly over decades, but its cumulative effect can be substantial.
Several factors may contribute to age-related muscle loss including reduced protein synthesis, hormonal changes, decreased physical activity, chronic low-grade inflammation, and reduced nerve function to muscles. While some degree of muscle loss appears to accompany aging, research suggests the rate and extent can be significantly influenced by lifestyle factors.
What makes this particularly concerning for body composition is that muscle loss often occurs alongside fat gain. Even if weight remains stable, the body's composition shifts toward less muscle and more fat, which is fundamentally altering metabolic health and your physical function.
Body recomposition refers to simultaneously losing fat mass while maintaining or gaining muscle mass. This represents a fundamentally different approach than simple weight loss, which often results in losing both fat and muscle.
This requires a significant mindset shift for many people. We're conditioned to view the scale as the primary measure of progress. Weight going down feels like success. Weight staying the same feels like failure. But with body recomposition, the scale might not move at all, even as your body undergoes profound positive changes.
You might gain five pounds of muscle and lose five pounds of fat. The scale shows zero change. But your body composition has improved dramatically. Your metabolism is more efficient. Your strength has increased. Your disease risk has decreased. Your clothes fit differently. You look and feel different. But the number on the scale tells none of that story.
This is why shifting focus from weight to body composition can be psychologically challenging but critically important. In this scenario, progress isn't measured by pounds lost. It's measured by how your body is changing in composition, how your strength is improving, how your metabolic markers are shifting, and how your functional capacity is increasing.
The Body Recomposition Approach
Improving body composition means increasing muscle while decreasing fat. This could look different for different people: some may lose fat while keeping their muscle, and others may gain muscle while losing fat.
The scale might show minimal change or even an increase in weight during successful body recomposition, particularly when muscle is being gained. This is why tracking body composition in addition to weight can give you a fuller understanding of your health progress.
Visceral Fat vs. Subcutaneous Fat
Not all fat tissue has the same health implications. Subcutaneous fat (stored under the skin) appears to be relatively metabolically neutral. Visceral fat (which accumulates around internal organs in the abdominal cavity) tends to be more metabolically active and is associated with increased risk of metabolic dysfunction (such as elevated blood sugar, high triglycerides, and altered cholesterol levels), insulin resistance, and cardiovascular disease.
Body recomposition that reduces visceral fat while maintaining or building muscle can lead to substantial health improvements even if total weight doesn't change significantly.
Several evidence-based approaches can help optimize body composition, though responses vary by individual.
Resistance Training
This probably doesn't come as a surprise, but progressive resistance training appears to be the most effective method for building and maintaining muscle mass. This includes lifting weights, bodyweight exercises, or resistance bands that progressively challenge muscles over time.
Key principles that may support muscle development include training each major muscle group at least twice per week. A common and effective split includes push exercises (chest, shoulders, triceps), pull exercises (back, biceps), and legs (quadriceps, hamstrings, glutes, calves). You'll also want to use sufficient resistance to challenge muscles within 8 to 15 repetitions, progressively increase weight or resistance over time, and allow adequate recovery between workouts.
Studies suggest that resistance training can help preserve or increase muscle mass even during caloric restriction, making it particularly important for body recomposition.
Adequate Protein Intake
Protein provides the amino acids necessary for muscle protein synthesis. Research suggests that protein requirements may be higher for older adults and those engaging in regular resistance training compared to sedentary younger adults.
Current evidence suggests that protein intakes in the range of 0.7 to 1.0 grams per pound of body weight per day (approximately 1.6 to 2.2 grams per kilogram) may support muscle maintenance and growth, particularly when combined with resistance training. Distributing protein intake relatively evenly across meals, rather than concentrating it in one meal, may also be beneficial.
Good protein sources include lean meats, poultry, fish, eggs, and dairy products. For plant-based options, combining foods like beans with rice, or quinoa with legumes can provide complete amino acid profiles.

Quality Sleep and Recovery
Sleep appears to play an important role in muscle recovery and growth. During sleep, the body releases growth hormone and undergoes repair processes that may support muscle protein synthesis.
Research suggests that inadequate sleep or poor sleep quality may be associated with increased muscle loss, reduced recovery from training, and impaired body composition. Prioritizing 7 to 9 hours of quality sleep can support body recomposition efforts.
Managing Stress and Inflammation
Chronic stress and elevated cortisol levels may be associated with muscle breakdown and increased fat storage, particularly visceral fat. Chronic low-grade inflammation may also interfere with muscle protein synthesis and contribute to muscle loss.
Stress management approaches such as meditation, adequate recovery time, and addressing sources of chronic stress may support better body composition outcomes.
Caloric Considerations
While body recomposition can occur at weight maintenance calories, particularly in individuals new to training, some people may benefit from a modest caloric deficit if fat loss is a primary goal. However, deficits should generally be moderate to help preserve muscle mass.
Very large caloric deficits, especially without adequate protein and resistance training, tend to result in greater muscle loss alongside fat loss. A more moderate approach that prioritizes protein intake and resistance training may support better body composition outcomes.
Unlike weight, which can be easily measured on a home scale, body composition requires different assessment methods. DEXA scans (which measure muscle, fat, and bone density), bioelectrical impedance analysis (BIA) available in some gyms and clinics, bod pod or hydrostatic weighing, and skinfold measurements performed by trained practitioners are some of the few methods that can provide accurate body composition measurements.
If a DEXA scan isn't accessible or affordable, consider these alternatives: many gyms and fitness centers offer BIA measurements or skinfold caliper testing at low cost. Some smart scales with BIA technology can track trends over time, even if absolute accuracy varies. Progress photos taken under consistent lighting and angles can reveal body composition changes the scale misses. How your clothes fit, particularly around the waist and shoulders, can also indicate whether you're losing fat and maintaining or gaining muscle. Strength improvements in the gym (lifting heavier weights over time) often correlate with muscle maintenance or growth.
Body composition matters differently at each stage of life. In your 20s and 30s, the muscle you build can help create a metabolic and functional reserve that protects you decades later. During your 40s and 50s, preservation becomes critical as natural age-related decline accelerates, making resistance training and adequate protein essential for preventing the muscle loss many assume is inevitable. For those in their 60s and beyond, muscle mass and strength become directly connected to independence and quality of life. Greater muscle in older age is associated with reduced disability, better metabolic health, lower fall risk, and potentially longer life. The difference between independent living and requiring assistance often comes down to whether adequate muscle mass has been preserved.
The strategies that support healthy body composition remain largely the same across all ages. They work together to support not just the balance between muscle and fat, but your overall capacity to live well and independently. Progress isn't always visible in pounds. Often, the most important changes are the ones the scale can't measure.

